Depression does not manifest itself in the manner that people anticipate. It is sometimes as though fatigue never wears out completely. It is losing interest in things that once mattered sometimes. And other times, it is just being uncharacteristically out of shape the whole time without knowing why. Many people try therapy. Many try medication. Some feel better for a while. Other people do not change significantly. As soon as it occurs, one may start thinking whether anything will actually help. Here is where Transcranial Magnetic Stimulation (TMS Treatment Help) has come into play as a significant alternative for those who feel stuck. Not as a miracle cure. Not to substitute all the rest of it. However, as an alternative solution, particularly when combined with the use of Integrative Psychiatry Services, General Psychiatry Treatment, Anxiety Disorder Therapy, and a qualified Depression Treatment Specialist. Now let us discuss TMS plainly and straightforwardly, what it is, who it is useful for, and why it can really do well in the life of the right individual.
Depression Isn’t Just Emotional It’s Neurological
The greatest misconception with depression is the perception that it is only emotional or psychological. In an actual sense, depression alters the functioning of the brain. Individuals who have to cope with depression usually talk about: Experiencing mental slowness. Difficulty beginning any easy tasks. Lacking a connection with emotions. Constant mental fatigue Poor concentration or remembering ability. This is the reason why General Psychiatry Treatment is not only concerned with talk therapy, but also the functioning of brain chemistry and brain activity. In some cases of the brain where some parts are not functioning well, there is no benefit in trying hard to overcome it. It is where such treatments as TMS are applicable.
What TMS Treatment Really Is (Without the Jargon)
TMS stands for Transcranial Magnetic Stimulation. Despite the complicated name, the concept is fairly simple.
TMS uses magnetic pulses to gently stimulate specific areas of the brain that are known to be involved in mood regulation. These areas are often less active in people with depression.
What makes TMS different:
- It’s non-invasive
- It doesn’t involve medication
- It targets the brain directly
- There’s no downtime after sessions
For many patients already receiving Integrative Psychiatry Services, TMS fits naturally into a broader care plan instead of replacing it.
How TMS Helps Reduce Depression Symptoms Over Time
Depression often involves disrupted communication between brain cells. Certain pathways don’t fire the way they should. Over time, this affects mood, motivation, and emotional resilience.
TMS works by encouraging healthier brain activity patterns. With repeated sessions, the brain begins to respond differently—not overnight, but gradually.
Patients often report:
- Feeling emotionally “lighter.”
- Having more mental clarity
- Finding it easier to get through the day
- Feeling less overwhelmed by small things
A Depression Treatment Specialist monitors this progress closely and adjusts treatment as needed, which is a big reason outcomes tend to be better with personalized care.
Why Integrative Psychiatry Services Matter So Much
TMS is powerful, but it’s not meant to work alone. Integrative Psychiatry Services look at mental health from multiple angles at the same time.
This approach may include:
- Medication management (if appropriate)
- Psychotherapy
- Lifestyle and stress evaluation
- Advanced treatments like TMS
Instead of asking, “What’s the one solution?” integrative care asks, “What combination will work best for this person?”
That mindset is often what makes long-term improvement possible.
The Importance of Working With a Depression Treatment Specialist
TMS isn’t something that should be rushed or applied automatically. A skilled Depression Treatment Specialist takes the time to understand the full picture.
They look at:
- Treatment history
- Response to medications
- Co-existing anxiety symptoms
- Daily functioning and stress levels
This ensures TMS is used thoughtfully and safely—not as a last-ditch effort, but as a strategic part of care.
Depression and Anxiety Often Overlap
It’s extremely common for depression and anxiety to exist together. Many patients feel low and exhausted while also feeling tense, worried, or restless.
While TMS is most commonly associated with depression, many people notice improvements in anxiety symptoms as well—especially when they’re also participating in Anxiety Disorder Therapy.
Some reported benefits include:
- Feeling less emotionally reactive
- Improved sleep
- Easier participation in therapy
- Better stress tolerance
When Anxiety Disorder Therapy and TMS support each other, progress often feels more balanced and stable.

What TMS Sessions Are Actually Like
People often imagine TMS as intense or uncomfortable. In reality, sessions are quite straightforward.
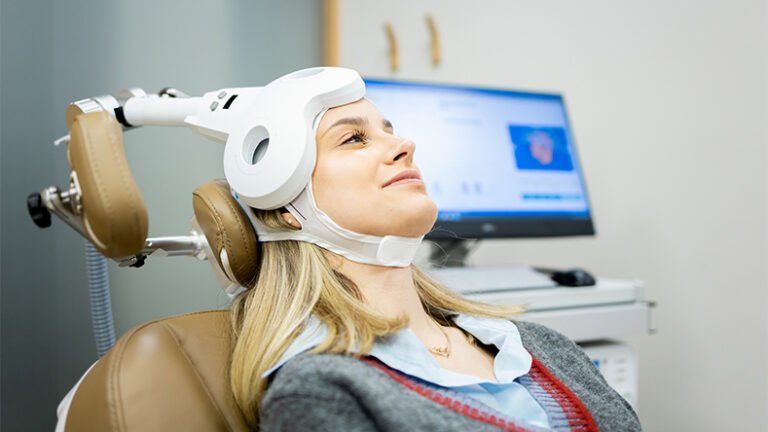
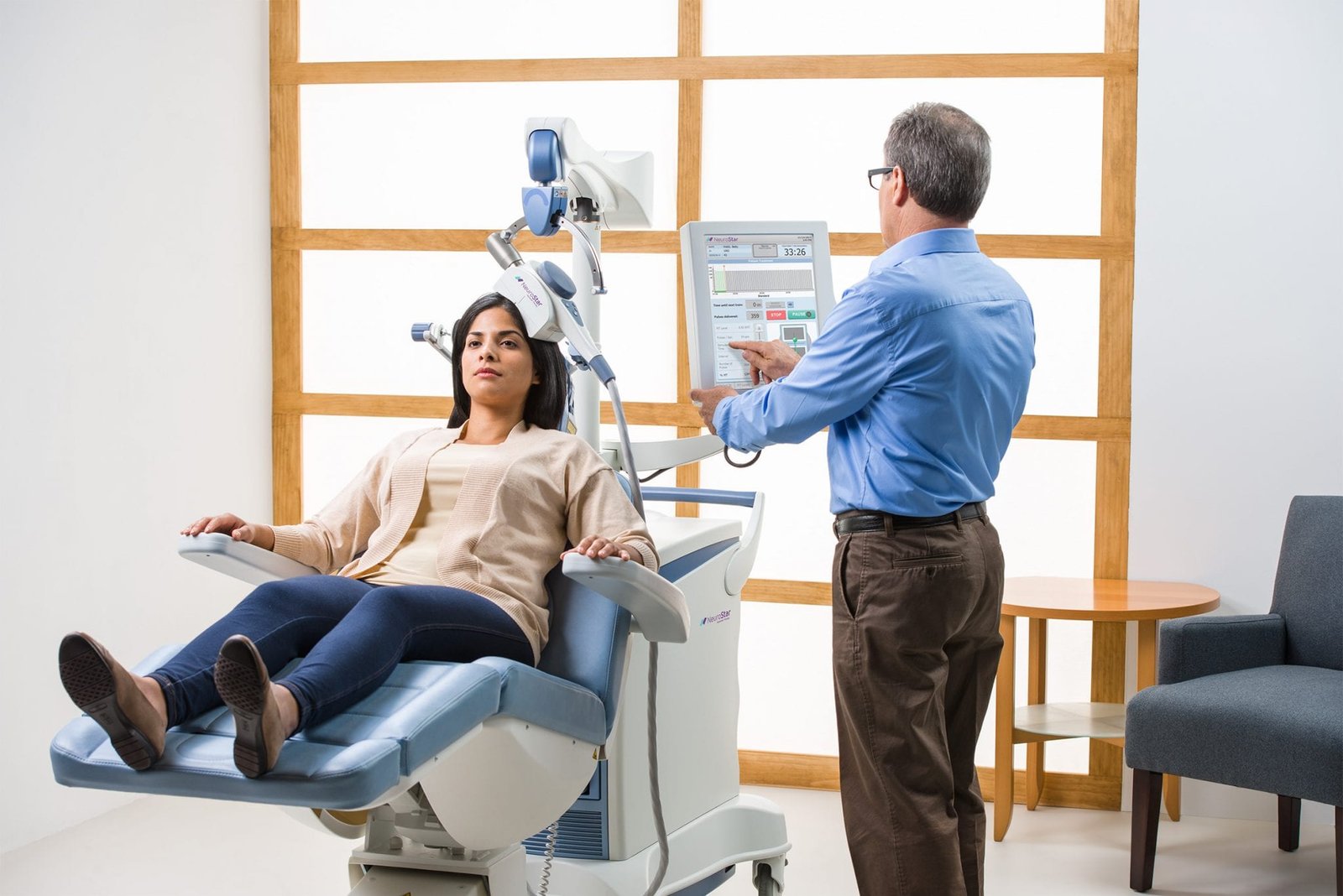
During a session:
- You sit comfortably in a chair
- A small device rests against your head
- Magnetic pulses are delivered
- Sessions last around 20–40 minutes
There’s no sedation. No recovery time. Most people go back to work or daily activities immediately afterward.
Safety and Side Effects An Honest Look
One reason TMS has become more common in General Psychiatry Treatment is its safety profile.
Most side effects are mild and temporary, such as:
- Slight scalp discomfort
- Mild headaches
- Sensitivity during early sessions
Serious side effects are rare, especially when treatment is guided by an experienced Depression Treatment Specialist.
When Do People Usually Start Feeling Better?
TMS works gradually. Most treatment plans involve several weeks of consistent sessions.
Many people notice changes such as:
- Improved emotional stability
- More energy
- Better focus
- Less emotional heaviness
When supported by Integrative Psychiatry Services, these improvements often continue even after treatment ends.
Who TMS Is Often Best Suited For
TMS may be a good option for people who:
- Have tried multiple treatments without lasting results
- Experience medication side effects
- Want a non-medication option
- Are already engaged in General Psychiatry Treatment
A full psychiatric evaluation helps determine whether TMS is appropriate for each individual.
Why TMS and Therapy Work Better Together
TMS helps the brain function more effectively. Therapy helps people understand thoughts, emotions, and patterns. Together, they reinforce each other.
This combination helps patients:
- Build coping skills
- Improve emotional insight
- Reduce relapse risk
- Maintain progress
This layered approach is a core part of effective Integrative Psychiatry Services.
Final Thoughts: A Realistic Path Forward
Depression may end up isolating and discouraging people, more so when their treatments may not yield as expected. TMS does not represent a miracle, but it is a significant turning point for many people. TMS can be used in combination with General Psychiatry Treatment, Anxiety Disorder Therapy, and individualized Integrative Psychiatry Services, providing an evidence-based, practical means to proceed to permanent progression. When considering the higher end of mental health care treatment, BleyanPsych is dedicated to thoughtful, personalized treatment tailored towards the real person and not the one-size-fits-all type.
For more updates and details, visit our Instagram Page!
FAQs
1. Is TMS uncomfortable?
Most people describe mild discomfort that usually improves after the first few sessions.
2. Can TMS help if medication didn’t?
Yes. Many people who haven’t responded well to medication benefit from TMS under care of a Depression Treatment Specialist.
3. How does TMS fit into integrative care?
It complements therapy, medication management, and lifestyle support within Integrative Psychiatry Services.
4. Does TMS help anxiety too?
Many patients report reduced anxiety, especially when combined with Anxiety Disorder Therapy.
5. How do I know if TMS is right for me?
A full evaluation through General Psychiatry Treatment is the best way to determine suitability.

No comment