Treatment of mental health has been taken to a different level. In the modern world, individuals desire more specific, science-based, and yet highly human care. That is where Transcranial Magnetic Stimulation (TMS) and integrative mental health methods meet. A common question that most patients seekingIntegrative psychiatry Services pose is: Why, exactly, is TMS measured and how does it apply in a comprehensive psychiatric care plan? This insight could make you feel more confident, informed and empowered in your treatment journey. Within this comprehensive guide, we will deconstruct the measurement of TMS, the mechanisms of TMS in integrative psychiatry, and the reason why it increasingly incorporates TMS along with General Psychiatry Treatment, Anxiety Disorder Therapy, and treatment with a depression treatment specialist. We will explain it in an easy, common-sense manner, most importantly, with no jargon or confusion.
What Is TMS and Why Does It Matter in Modern Psychiatry?
Transcranial Magnetic Stimulation (TMS) is a non-invasive therapy that uses targeted magnetic pulses to stimulate specific areas of the brain involved in mood regulation, focus, and emotional processing.
Unlike medications, TMS does not circulate through the bloodstream. Instead, it directly influences neural pathways linked to depression, anxiety, and other mood disorders.
In Integrative Psychiatry Services, TMS is not viewed as a standalone miracle solution. It’s a tool one that works best when combined with therapy, lifestyle support, and personalized psychiatric care.
Key reasons TMS is gaining attention:
- Non-invasive and drug-free
- No anesthesia or sedation required
- Minimal systemic side effects
- Backed by growing clinical research
This makes it especially valuable within General Psychiatry Treatment plans designed for patients who haven’t found full relief through medication alone.
How Is TMS Measured? Understanding the Science Behind Precision
One of the most important aspects of TMS therapy is accurate measurement. Precision ensures that treatment is safe, effective, and tailored to each individual brain.
Motor Threshold: The Foundation of TMS Measurement
TMS measurement begins with identifying the motor threshold (MT). This is the minimum magnetic intensity required to stimulate a motor response, typically observed as a small movement in the hand or fingers.
Why this matters:
- Everyone’s brain responds differently to stimulation
- The motor threshold helps personalize treatment intensity
- It reduces the risk of overstimulation or under-treatment
By calculating the motor threshold, clinicians can adjust the magnetic pulses to an optimal level—strong enough to activate targeted brain regions but still safe and comfortable.
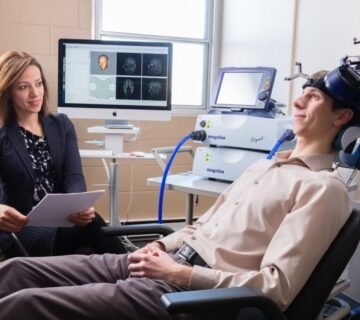
Brain Mapping for Targeted Accuracy
After determining the motor threshold, clinicians perform brain mapping to locate the exact region associated with mood regulation—most often the left dorsolateral prefrontal cortex.
This mapping process:
- Ensures consistent coil placement
- Improves treatment reliability
- Allows for precise repetition across sessions
In Integrative Psychiatry Services, this level of customization reflects a broader commitment to personalized care rather than generic protocols.
How TMS Sessions Are Structured and Monitored
TMS is not a single-session treatment. It’s a structured course designed to create lasting changes in brain activity over time.
Typical TMS Treatment Structure
Most patients undergo:
- 4–5 sessions per week
- Sessions lasting 20–40 minutes
- A treatment course of 4–6 weeks
Throughout the process, clinicians closely monitor progress and comfort levels.
Tracking Progress During Treatment
Progress is measured using:
- Clinical symptom scales
- Patient self-reports
- Behavioral and mood changes
- Ongoing psychiatric evaluations
This continuous feedback loop allows providers offering General Psychiatry Treatment to adjust care plans as needed—whether that means refining TMS settings, adding therapy sessions, or modifying medications.
The Role of TMS in Integrative Psychiatry Care
Integrative psychiatry looks at the full picture of mental health—biological, psychological, and lifestyle factors included. TMS fits naturally into this model because it addresses brain function directly while supporting broader treatment goals.
TMS as Part of a Whole-Person Approach
Within Integrative Psychiatry Services, TMS is often combined with:
- Psychotherapy and counseling
- Medication management
- Nutritional and lifestyle guidance
- Stress regulation techniques
This approach acknowledges that lasting mental wellness doesn’t come from a single intervention—it comes from coordinated care.
Using TMS Alongside General Psychiatry Treatment
TMS is frequently introduced when traditional General Psychiatry Treatment hasn’t provided sufficient relief. That doesn’t mean medications or therapy are abandoned.
Instead, TMS often:
- Enhances medication response
- Allows for lower medication dosages
- Reduces medication-related side effects
- Supports cognitive and emotional regulation
This makes it a valuable option for patients seeking progress without constantly switching prescriptions.

TMS and Anxiety Disorder Therapy: What to Know
While TMS is widely recognized for depression, it is increasingly used within Anxiety Disorder Therapy as well.
How TMS Supports Anxiety Treatment
TMS may help by:
- Regulating overactive neural circuits
- Improving emotional control
- Reducing physical symptoms of anxiety
- Enhancing therapy outcomes
When integrated with psychotherapy and coping strategies, TMS can strengthen the overall effectiveness of Anxiety Disorder Therapy, especially for individuals with treatment-resistant symptoms.
The Role of a Depression Treatment Specialist in TMS Care
TMS is most effective when guided by a qualified Depression Treatment Specialist who understands both the science and the individual.
Why Specialist Oversight Matters
A dedicated specialist:
- Evaluates whether TMS is appropriate
- Interprets symptom changes accurately
- Coordinates TMS with other treatments
- Adjusts care based on patient response
This expertise ensures that TMS is not used in isolation, but as part of a thoughtful, results-driven treatment plan.
Measuring Success: How Clinicians Evaluate TMS Outcomes
Success in TMS therapy isn’t defined by one single factor. Instead, clinicians look at a combination of measurable improvements.
Common Indicators of Progress
- Reduced depressive symptoms
- Improved mood stability
- Better sleep patterns
- Increased motivation and focus
- Improved quality of life
Within Integrative Psychiatry Services, success also includes how well patients function in daily life—not just how they score on clinical scales.
Is TMS Right for Everyone?
TMS is not a universal solution, and integrative psychiatry emphasizes informed decision-making.
Ideal Candidates for TMS May Include:
- Individuals with treatment-resistant depression
- Patients experiencing medication side effects
- Those seeking non-invasive options
- People working with a Depression Treatment Specialist for long-term care
A thorough psychiatric evaluation is always essential before starting treatment.
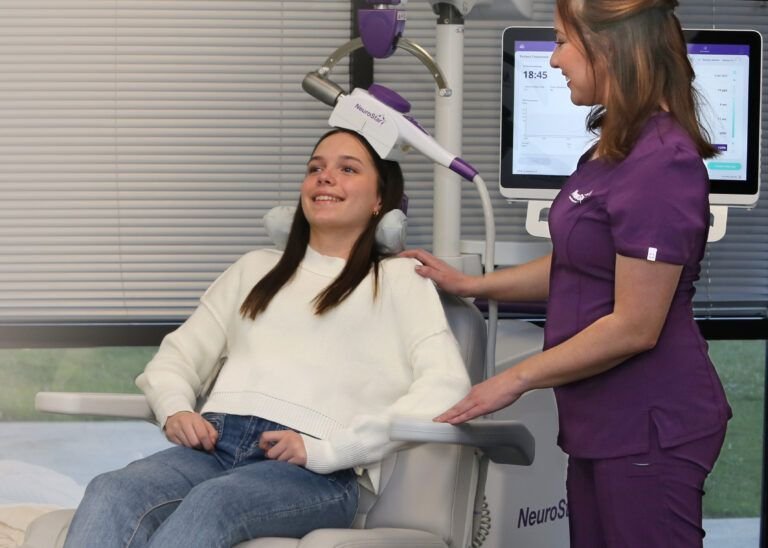
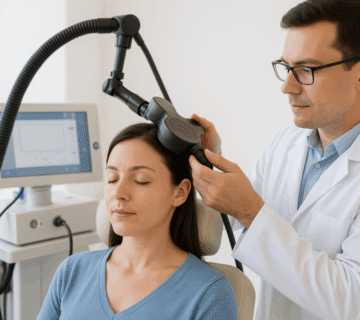
The Patient Experience: What TMS Actually Feels Like
One common concern is whether TMS is uncomfortable or intimidating.
Most patients describe:
- A tapping sensation on the scalp
- Mild discomfort that fades quickly
- No downtime after sessions
- Ability to return to normal activities immediately
This ease of use makes TMS compatible with busy lifestyles and ongoing General Psychiatry Treatment plans.
Why Integrative Psychiatry Is Shaping the Future of Mental Health
Mental health care is shifting toward personalization, collaboration, and long-term wellness. Integrative Psychiatry Services reflect this change by combining advanced treatments like TMS with human-centered care.
Rather than focusing solely on symptom suppression, integrative psychiatry aims to:
- Restore brain balance
- Build emotional resilience
- Support sustainable mental wellness
TMS is one piece of this larger, forward-thinking approach.

Conclusion: Moving Forward with Confidence and Clarity
Understanding how TMS is measured and used in integrative psychiatry empowers you to make informed decisions about your mental health care. From precise motor threshold measurements to personalized treatment planning, TMS represents a thoughtful blend of technology and compassion.
When combined with General Psychiatry Treatment, Anxiety Disorder Therapy, and expert guidance from a Depression Treatment Specialist, TMS becomes more than a procedure it becomes part of a holistic path toward healing.
If you’re exploring advanced mental health options, working with a trusted integrative care provider like bleyanpsych can help you determine whether TMS fits your unique needs.
For more updates and details, visit our Instagram Page!
Frequently Asked Questions (FAQs)
1. How long does it take to see results from TMS therapy?
Many patients notice gradual improvement within two to four weeks, though timelines vary. In Integrative Psychiatry Services, progress is monitored closely to ensure meaningful, lasting results.
2. Can TMS replace medication in general psychiatry treatment?
TMS does not automatically replace medication. It often works alongside General Psychiatry Treatment, and any medication changes should be guided by a qualified psychiatrist.
3. Is TMS effective for anxiety disorders?
TMS can support Anxiety Disorder Therapy, particularly when anxiety is linked to mood regulation issues. Outcomes improve when TMS is combined with therapy and lifestyle support.
4. How does a depression treatment specialist decide if TMS is right for me?
A Depression Treatment Specialist evaluates your symptoms, treatment history, and overall mental health to determine whether TMS is appropriate and how it should be integrated.
5. Are the effects of TMS permanent?
Results can be long-lasting, especially when supported by ongoing Integrative Psychiatry Services. Some patients may benefit from maintenance sessions depending on individual needs.

No comment