When someone starts Transcranial Magnetic Stimulation (TMS) Treatment, the first question is often simple: Will it work for me? That is a fair concern, especially for people who have already tried medication, talk therapy, or both without getting enough relief. Personalized Integrative Psychiatry looks at the whole person—mind, body, and lifestyle—to understand why certain treatments may not have worked before. TMS has become an important option for treatment-resistant depression, and it is also used for some other mental health conditions in selected cases. It is noninvasive and does not require surgery or sedation, and when combined with Personalized Integrative Psychiatry, it may help create a more tailored and effective treatment plan for better mental health outcomes.
But here is where the conversation gets more interesting. TMS does not happen in a vacuum. Many patients do better when brain-based treatment is paired with a broader, more individualized plan that looks at sleep, stress, nutrition, medical history, medications, therapy needs, and the patterns driving symptoms. That is exactly where Personalized Integrative Psychiatry can add value. Rather than replacing evidence-based psychiatry, it builds on it with a more complete view of the person.
For a practice focused on Integrative Psychiatry Services, this matters. Patients seeking help for depression, anxiety, OCD, or complex mood symptoms are often not looking for a one-size-fits-all solution. They want care that feels precise, thoughtful, and responsive. In that setting, combining General Psychiatry Treatment with TMS and supportive integrative strategies can strengthen engagement, improve consistency, and address factors that may otherwise limit progress.
What does Personalized Integrative Psychiatry actually mean?
At its core, Personalized Integrative Psychiatry means building treatment around the patient rather than forcing the patient into a rigid treatment template. It typically combines standard psychiatric tools such as diagnosis, medication management, and psychotherapy referrals with complementary strategies like lifestyle review, mind-body practices, nutrition-focused guidance, and careful evaluation of contributing health factors. The goal is not to chase trends. It is to use clinically appropriate, evidence-informed options in a coordinated way.
That kind of approach is especially relevant in modern mental health care because symptoms rarely have just one driver. A patient with depression may also have chronic insomnia, high stress, medication sensitivity, nutritional issues, unresolved trauma, or obsessive thought patterns. A patient pursuing Anxiety Disorder Therapy may also need medication adjustment, sleep stabilization, and structured coping tools. Integrative psychiatry tries to connect those dots instead of treating each symptom in isolation.
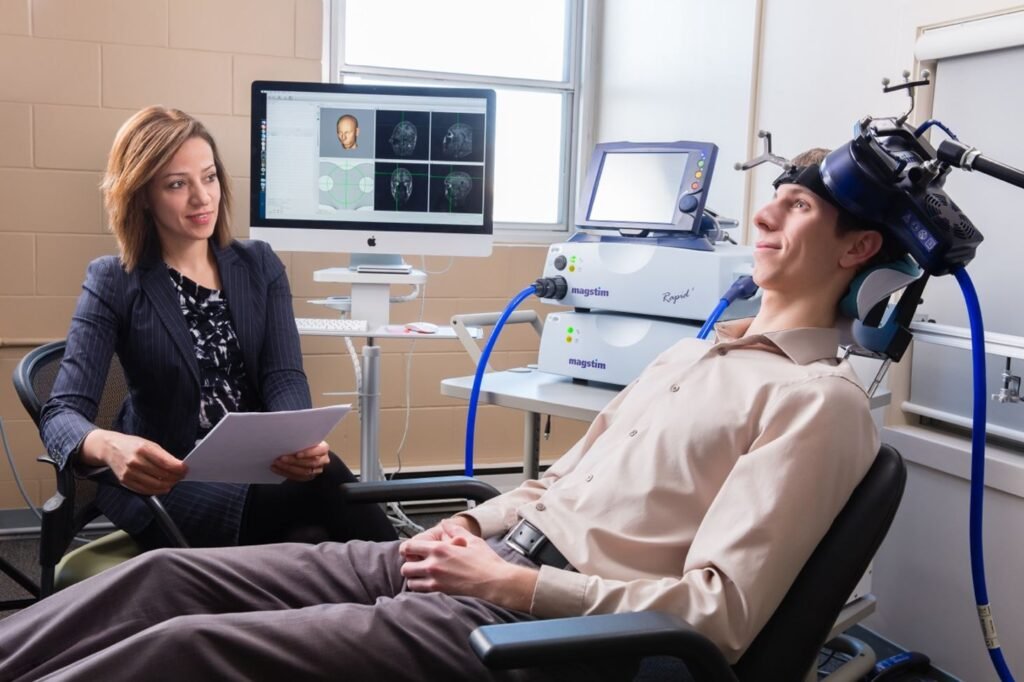
Why TMS often works best as part of a larger treatment plan
TMS is designed to stimulate specific brain regions involved in mood regulation. It is FDA-cleared for major depression, and reputable medical sources describe it as an option when other depression treatments have not worked well enough. More recent clinical literature also continues to support its safety and effectiveness for depression, while newer protocols are expanding how it is delivered.
Still, even a strong treatment can underperform if the surrounding care is fragmented. A person receiving TMS while sleeping poorly, skipping follow-up, taking poorly tolerated medication, or feeling overwhelmed by untreated anxiety may not get the same overall outcome as someone whose full care plan is coordinated. That does not mean TMS fails. It means response can be influenced by what else is happening in the patient’s mental and physical health landscape. This is a clinical inference based on how integrated care is designed to improve coordination and outcomes.
How Integrative Psychiatry Services can enhance TMS effectiveness
1. Better patient selection from the start
Not every patient needs the same intervention at the same time. A thorough psychiatric evaluation can clarify whether TMS is the right next step, whether depression is primary, and whether other concerns, such as OCD symptoms, trauma, personality-related patterns, or substance use are also shaping the presentation. Better diagnostic clarity often leads to better sequencing of care.
2. Stronger day-to-day symptom support
TMS sessions happen on a schedule, but symptoms show up every day. Patients may still need help with panic, rumination, irritability, low motivation, intrusive thoughts, or poor sleep while TMS is underway. This is where General Psychiatry Treatment, medication review, psychotherapy coordination, and practical coping strategies become essential. They support the patient between sessions and reduce the chance that TMS is expected to carry the full burden alone.
3. A more complete depression strategy
A good Depression Treatment Specialist does more than confirm a diagnosis. They look for the patterns that keep depression stuck. That may include chronic stress, incomplete prior treatment, low adherence, sleep problems, coexisting anxiety, or obsessive-compulsive symptoms. When those barriers are addressed alongside TMS, the overall treatment plan becomes more coherent and more realistic for the patient to follow.
4. Thoughtful use of supplements and lifestyle guidance
Many patients ask about Supplements for Mental Wellness, mental wellness supplements, or even “what are the best supplements for mental health.” That interest is understandable, but this is an area where caution matters. The NCCIH notes that some complementary approaches may help in certain situations, but evidence varies, and these options should not be treated as automatic substitutes for standard care. In real practice, supplements should be selected only when clinically appropriate and with attention to interactions, diagnosis, and treatment goals.
That means articles and treatment pages should avoid promising that any single mental health supplement, “reacted iron supplement,” or “best vitamins for mental health” will make TMS work better for everyone. A safer and more credible message is this: carefully supervised lifestyle and supplement strategies may support overall mental wellness for some patients, but they should be individualized and medically reviewed.
5. Better care for complex conditions
Patients seeking TMS may also need support for anxiety, trauma, or Obsessive Compulsive Disorder (OCD) Care. Even when TMS is being used mainly for depression, coexisting symptoms can shape how treatment feels and how progress is measured. Integrative care helps clinicians account for those layers instead of focusing too narrowly on a single symptom score.
Holistic TMS Care is not “alternative” care
One common misunderstanding is that integrative psychiatry means replacing evidence-based medicine with wellness trends. That is not what responsible integrative care looks like. The best version of it is grounded, structured, and medically supervised. It starts with standard psychiatry and adds supportive tools that fit the patient’s diagnosis, preferences, and response patterns.
That is why Holistic TMS Care can be such a strong content angle for this topic. It speaks to what many patients actually want: advanced treatment that still feels personal. It also fits search intent well, because people researching TMS often want both effectiveness and a fuller plan for recovery. Used naturally, Holistic TMS Care helps connect TMS with real-world clinical support rather than presenting it as a standalone fix.
What patients usually want to know before starting TMS
Many prospective patients are not just comparing treatments. They are trying to understand the experience. Will it fit into work and family life? Will they need medication too? Should they continue therapy? Can anxiety or OCD symptoms be addressed at the same time? These are practical questions, and they are part of what makes Psychiatrist in Coral Springs FL, and psychiatry Coral Springs FL, searches so intent-driven. People are not only seeking information. They are looking for coordinated care.
For a local practice, that means content should reflect both expertise and reassurance. A page or article about TMS performs better when it explains not only what TMS is, but how it fits into broader mental health care in Coral Springs, including evaluation, therapy coordination, medication oversight, and individualized support. That local relevance also aligns naturally with search phrases like Coral Springs psychiatrist, psychiatrist in Coral Springs, psychiatrist Coral Springs FL, and depression treatment Coral Springs.
Practical ways an integrative psychiatrist can improve the TMS journey
Keep expectations realistic
TMS can be highly valuable, but patients still need honest guidance. Response may take time, and progress is not always linear. Clear communication improves trust and adherence.
Track more than one symptom
Mood matters, but so do sleep quality, anxiety, functioning, concentration, and intrusive thoughts. Broader tracking gives a more useful picture of recovery. This is particularly important when depression overlaps with OCD or anxiety.
Review the full treatment stack
Medication, therapy, nutrition habits, daily stress, and physical health all influence how supported a patient feels during TMS. Integrative care helps keep those pieces aligned.
Make room for individual differences
Some patients are looking for a child psychiatrist, some want adult medication management, and others want an insurance-friendly TMS center with a more personalized approach. Good psychiatry content should reflect those real variations in patient needs.
Mistakes people make when comparing TMS and integrative psychiatry
The first mistake is assuming they are competing options. They are not. TMS is a treatment modality, while integrative psychiatry is a care framework. One can strengthen the other. The second mistake is treating supplements as harmless add-ons that do not need psychiatric oversight. In reality, even seemingly simple supplements for mental health can be poorly matched, unnecessary, or incompatible with other parts of treatment.
The third mistake is focusing only on diagnosis labels and not on treatment barriers. Two people with depression may need very different plans depending on sleep, trauma history, anxiety severity, medication tolerance, and daily functioning. That is why Personalized Integrative Psychiatry is such a relevant framework for TMS-related care.
Holistic TMS Care in local psychiatric practice
For a practice associated with Diana Bleyan, Dr. Diana Bleyan, or Diana Bleyan MD, the strongest positioning is not simply offering TMS. It is offering TMS within a personalized psychiatric model that includes integrative evaluation, medication management where needed, psychotherapy coordination, and thoughtful discussion of lifestyle or supplement strategies when appropriate. Public profiles for the practice consistently describe a combination of general psychiatry, integrative psychiatry, TMS, psychotherapy, supplements, and mind-body wellness.
That combination supports a stronger patient message: advanced treatment, individualized planning, and compassionate follow-through. For readers searching for integrative psychiatry florida or a psychiatrist in Coral Springs FL, that is often more compelling than a generic description of TMS alone.

Final thoughts
So, can Integrative Psychiatry Services enhance the effectiveness of TMS therapy? In many cases, yes, not by replacing TMS, but by helping patients get more out of it. A personalized plan can improve diagnostic clarity, support adherence, address coexisting symptoms, and create a more complete recovery strategy. That is the real strength of Personalized Integrative Psychiatry: it treats TMS as part of a larger healing process, not a standalone event. For patients looking for a Depression Treatment Specialist, Anxiety Disorder Therapy, or a trusted Psychiatrist in Coral Springs FL, the most compelling message is simple: advanced treatment works best when it is also individualized. If your practice offers TMS alongside thoughtful integrative and general psychiatric care, that is not just a service list. It is a meaningful clinical advantage.
For more updates and details, visit our Instagram Page!
FAQs
Can integrative psychiatry replace TMS therapy?
Usually, no. Integrative psychiatry is better understood as a broader treatment approach, not a replacement for every evidence-based intervention. TMS may still be an excellent option for depression that has not responded adequately to standard treatment.
Does TMS help anxiety and OCD, too?
TMS is best known for depression, and some sources also note FDA approval or clinical use related to OCD in certain contexts. Whether it is appropriate depends on diagnosis, treatment history, and clinician evaluation.
Should I take supplements during TMS treatment?
Only with medical guidance. Some patients may benefit from targeted support, but supplements are not universally necessary, and evidence differs widely by product and condition.
Why combine General Psychiatry Treatment with TMS?
Because TMS addresses one important part of mental health care, while psychiatry also covers diagnosis, medication review, psychotherapy coordination, safety monitoring, and treatment planning. Combined care is often more practical and more patient-centered.
Is integrative psychiatry useful for depression only?
No. It may also be relevant for anxiety, sleep concerns, trauma-related symptoms, OCD-related care, and broader wellness planning, depending on the patient’s needs and the clinician’s scope of practice.



No comment